Posted
6th July 2022
Research
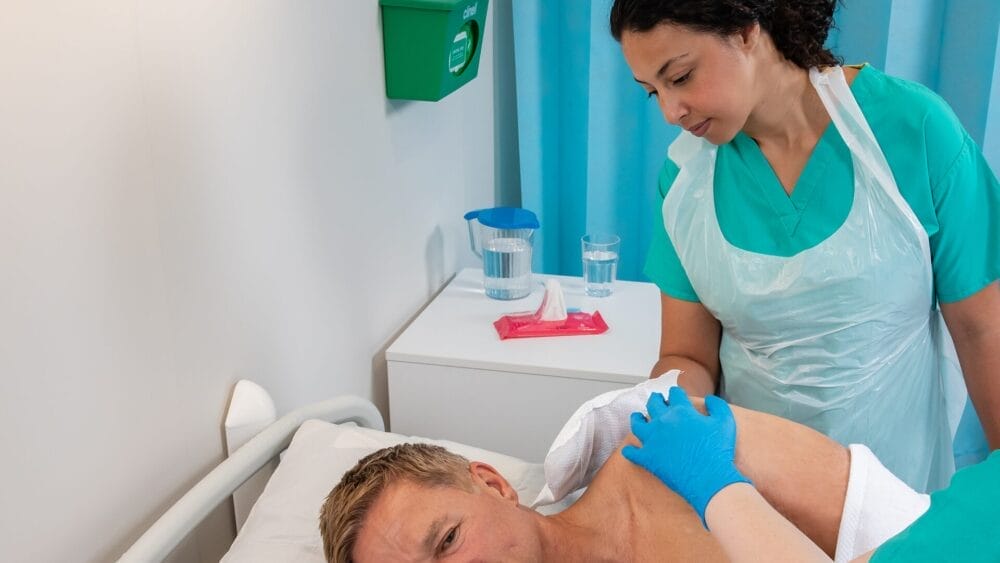
In today’s article, our Clinical Specialist for Capital, Claudia Santos, discusses air as a predominant route of transmission and how engineering can be utilised to minimise the spread and transmission of infections.
Looking back through the years, the link between engineering and environmental solutions and the resulting improvements in public health are very clear. The disease outbreaks in Roman military camps led to the development of public baths and aqueducts, whereas, more recently, the cholera epidemic of the 19th century led to the creation of sewage systems, which helped with the control of waterborne diseases such as cholera and typhoid.
So, why are we not treating air quality the same as water quality?
The main routes of transmission for diseases occur via water, direct physical contact, sexual or otherwise, and via the air. If air is such a predominant route of transmission for infections, then why are we not treating air quality like we do water quality? In fact, transmission is only one out of six aspects that form part of the chain of infection, with other links in the chain including microbial reservoir, portal of entry and exit and infectious agent.[1]
The chain of infection
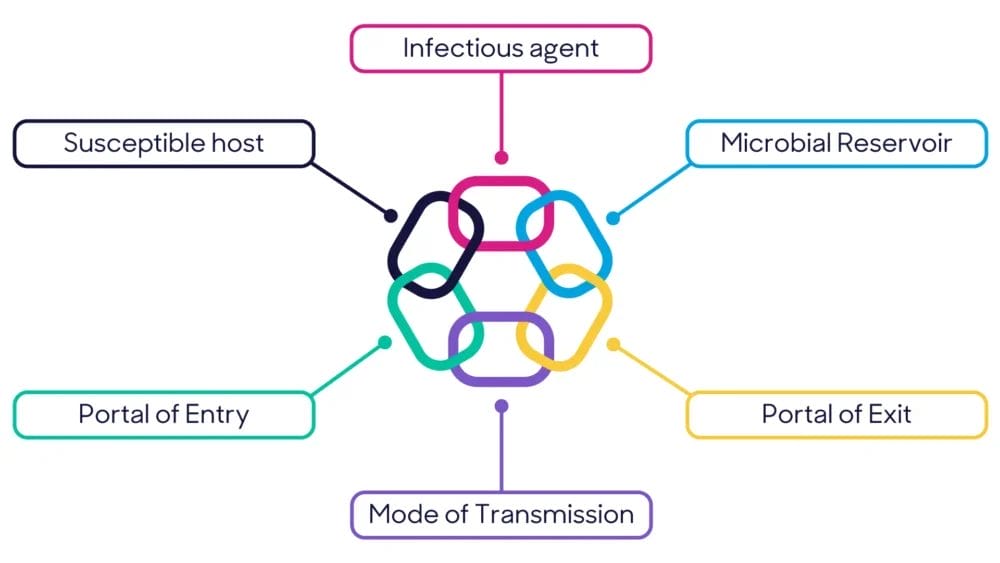
The chain of infection is used by many IPC teams, as well as public health professionals, to inform initiatives and measures relating to breaking the chain and hence stopping the spread of infection. If we take cholera as an example, infection prevention practices are related to the reservoir, in this case water, as well as portal of entry and exit. Ensuring access to clean water relates to the reservoir, whereas education around hand hygiene, sanitation and cooking, helps stop the spread of the disease from one host to another.[2]
Related article: Why taking care of the air makes our offices safer
How engineering can minimise the spread of infections
In March 2021, Sir Patrick Vallance, the prime minister’s Chief Scientific Advisor, commissioned the following report: Infection resilient environments: time for a major upgrade. The expert panel comprised some of the most respected individuals in the field of engineering and aimed to demonstrate how engineering and the built environment can be best utilised to minimise the spread and transmission of infections.
The report, written by a working group comprising members of the Royal Society of Engineering as well as the Chartered Institution of Building Services Engineers, highlighted that, if the “UK was to experience another pandemic in the next 60 years, not only would there be a societal cost, but the annual economic cost could reach £23 billion.” This statement was taken from a report conducted by NERA Economic Consulting who were commissioned by the RSE and used transmission and cost models, as well as literature reviews to undertake their report. This doesn’t consider the backlog of maintenance costs affecting the NHS, which according to the most recent report by NHS Digital totalled £9.2million.[3]
Related article: The importance of air filtration in dental rooms
How do we improve the current estates with an increasing pressure on hospital budget?
With a growing, ailing population and the need for additional, modern and fit for purpose hospitals, the time for ensuring that the relevant building regulations are applied has never been greater. The prime minister has announced a £3.7 billion package for the creation of 40 new hospitals by 2030,[4] much needed considering that 55% of Trusts do not comply with the HTM 03/01 standard, which focuses on specialised ventilation for healthcare.[5] But the question remains: how do we improve the current estates and facilities with an ever-increasing pressure on hospital budget and expenditure?
Related article: Why ventilation is important & the role of air filtration units
Rediair for instant air purification

A small study conducted in COVID-19 positive participants’ residences, showed that the use of portable air cleaners with HEPA filters resulted in a decrease in COVID-19 positive air samples.[6] Considering the financial implications of a complete overhaul of ventilation systems, which the report acknowledges might not be viable, the use of ‘hybrid ventilation’ or rather a mix of natural and mechanical ventilation could be an option and step in the right direction.
So with that, don’t you think that the air we breathe should be as clean as the water we drink?
If you’d like to find our more about air purification units, visit our Rediair page. Help spread the word about the importance of ventilation in healthcare by sharing this article on social media.
SHARE THIS ARTICLE
Tags
Latest News
Introducing HEXI HUB: A seamless transition in our product line
We’re pleased to announce an update to our product offering…
Innovative solutions for tackling Carbapenemase-producing Enterobacteriaceae (CPE) at King’s College Hospitals
King’s College Hospital NHS Foundation Trust, one of London’s largest…
Gloves Off: reducing unnecessary plastic waste during environmental cleaning and disinfection
In this blog, Dr Phil Norville discusses the momentum-gaining ‘Gloves…
Gloves Off: Navigating SDS sheets and skin safety claims in environmental decontamination products
In this blog, James Clarke (Head of R&D, Science &…