Posted
19th May 2017
Research
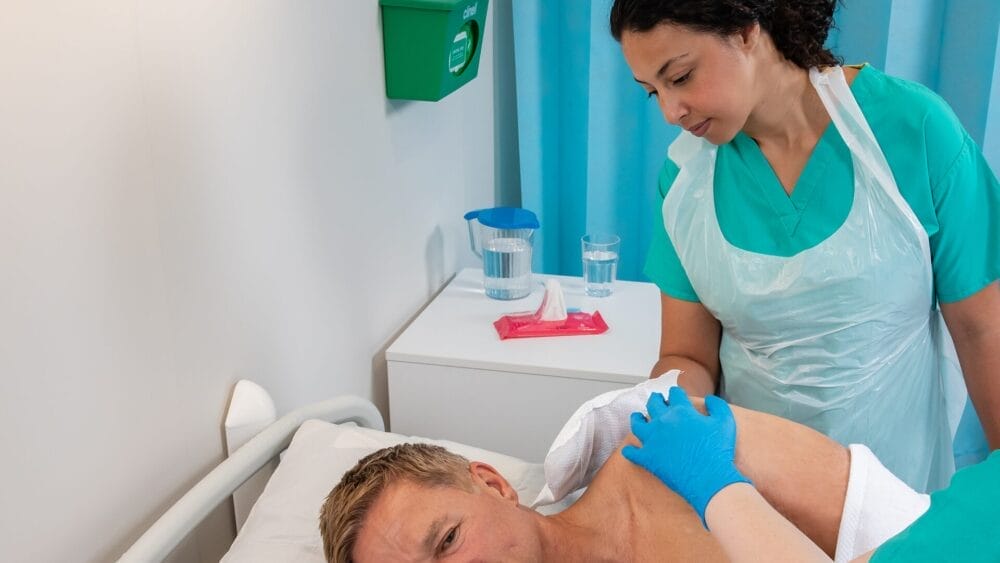
A helpful US study tracked the non-emergence of phenotypic or genotypic chlorhexidine resistance associated with hospital-wide use of chlorhexidine gluconate (CHG) antisepsis.
The 700 bed hospital introduced hospital wide CHG bathing in 2010, removed it in 2011, and reinstated it in 2015. They evaluated a collection of S. aureus isolates that were considered hospital-acquired and found that there was no reduction in CHG susceptibility during the two periods of CHG use, and found no evidence of qacA or qacB genes, which have been linked with reduced susceptibility to CHG. The study is one of the few that evaluated hospital-wide use of CHG, so there was certainly a pretty strong selective pressure for reduced susceptibility to emerge! Whilst this study does not prove that CHG is somehow ‘resistance-resistant’ – indeed, other studies have found evidence of reduced susceptibility associated with CHG use – it does reinforce that CHG is a well-tolerated antiseptic that does not readily promote reduced susceptibility.
SHARE THIS ARTICLE
Tags
Latest News
Introducing HEXI HUB: A seamless transition in our product line
We’re pleased to announce an update to our product offering…
Innovative solutions for tackling Carbapenemase-producing Enterobacteriaceae (CPE) at King’s College Hospitals
King’s College Hospital NHS Foundation Trust, one of London’s largest…
Gloves Off: reducing unnecessary plastic waste during environmental cleaning and disinfection
In this blog, Dr Phil Norville discusses the momentum-gaining ‘Gloves…
Gloves Off: Navigating SDS sheets and skin safety claims in environmental decontamination products
In this blog, James Clarke (Head of R&D, Science &…