Posted
21st September 2020
Research
This post shares the findings of a recent study exploring improving hospital cleaning and disinfection through streamlining product and enhanced training.
A team working in Lanarkshire, the third largest health board in Scotland, has recently published a study evaluating the impact of an intervention to improve hospital cleaning and disinfection through the implementation of pre-impregnated wipes combined with enhanced training. A survey of staff before and after the implementation identified significant benefits in terms of faster cleaning, and improved levels of training in staff doing the cleaning.
A survey of staff before and after the implementation identified significant benefits in terms of faster cleaning, and improved levels of training in staff doing the cleaning.
12 wards were chosen to participate in the study. Prior to the study, the hospitals were using detergent wipes and sodium hypochlorite as per standard Scottish national guidance. The intervention involved rationalising the products used for cleaning and disinfection to either a combined detergent/disinfectant wipe (Clinell Universal), and a sporicidal disinfectant wipe (Clinell Sporicidal). All staff working in the wards went through a training course specifically related to the use of the wipes and how to clean key items of equipment. Finally, some communications materials were launched to support good decision making around which wipe to use and how to use it correctly. A survey of the staff involved was undertaken before and after the interventions were implemented in order to evaluate impact.
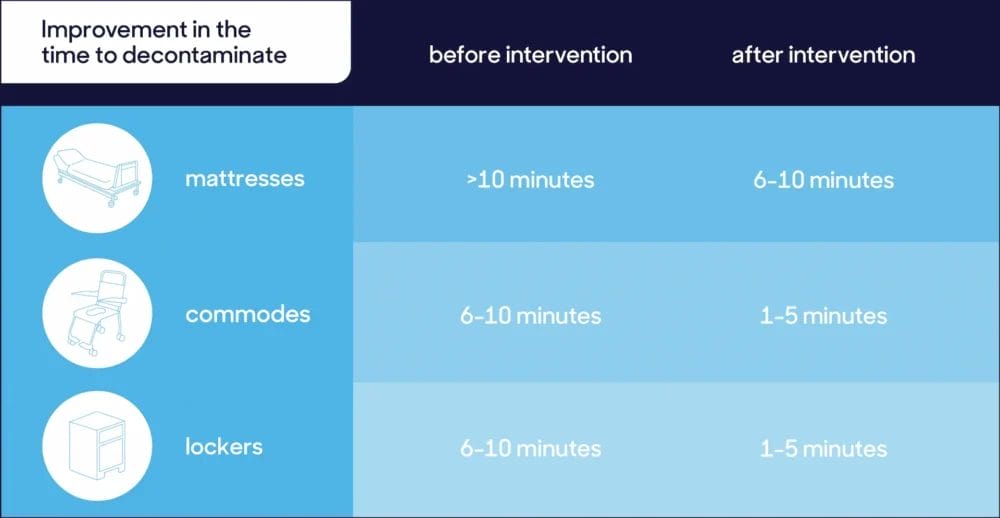
The surveys were completed by 120 healthcare workers before the intervention and 133 after the intervention. The survey demonstrated a significant improvement in the time to decontaminate mattresses (>10 mins before vs. 6-10 mins after), lockers (6-10 mins before vs. 1-5 mins after), and commodes (6-10 mins before vs. 1-5 mins after).
The survey also demonstrated a significant improvement in the proportion of healthcare workers who were trained for cleaning and disinfection, from 44% to 89% of staff in cleaning, 68% to 90% in non-sporicidal disinfection, and 40% to 89% in sporicidal disinfection.

Although not compared statistically, the survey also demonstrated improvements in the rationalisation of products recommended for cleaning and disinfection, a reduction in the amount of PPE and inappropriate PPE used, and the availability of the correct products at the point of use.
The study has several important limitations. For example, the study measured staff perceptions of the key outcomes (e.g. time to clean) rather than measuring the actual process time. And the intervention could not be blinded, so the presence of the IPC and study team may have influenced staff perceptions around the variables being measured.
Despite the limitations, the study demonstrates powerfully the impact of product rationalisation and training to improve the quality of hospital cleaning and disinfection in an acute care provider.
SHARE THIS ARTICLE
Tags
Latest News
GAMA Healthcare expands Rediroom fleet with additional order for Midlands Trust
GAMA Healthcare has secured an order for 8 more Redirooms,…
News from the front line: GAMA Healthcare partners with leading Midlands Trust to enhance air quality across two sites
GAMA Healthcare is pleased to announce a significant investment from…
Celebrating 20 Years of GAMA Healthcare: Our Story
This month, GAMA Healthcare celebrates 20 years of helping prevent…
Norovirus: Understanding its transmission and prevention in the UK
Introduction Norovirus is recognised as the leading cause of viral gastroenteritis…




