Posted
18th July 2023
Research
Candida auris is a key emerging threat to healthcare facilities worldwide. For reasons that are not completely clear, the prevalence of C. auris seems to be rising. C. auris is shed into the environmental, can survive on dry surfaces for extended periods, and there is evidence that surface contamination plays an important role of the transmission of C. auris in healthcare facilities.
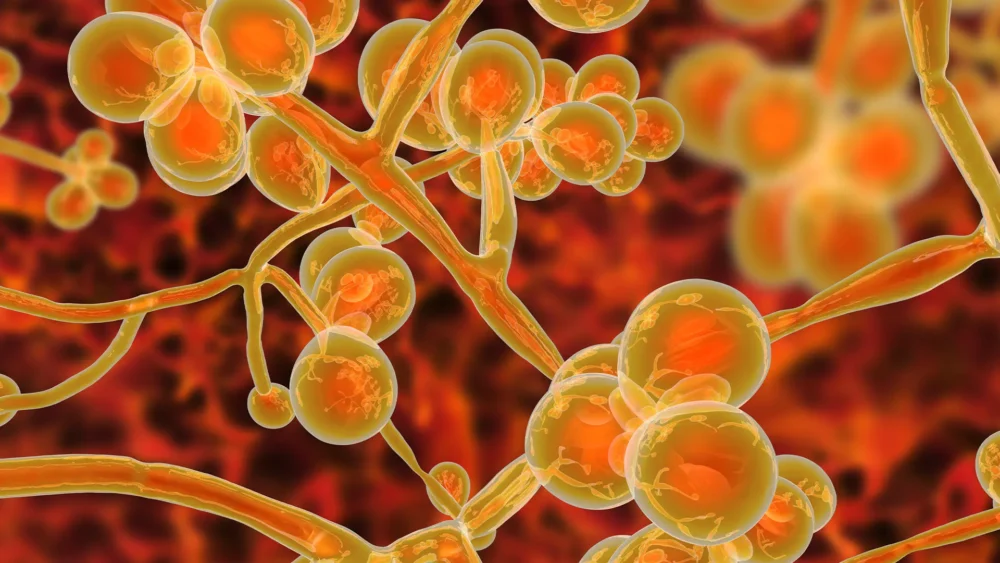
C. auris is a fungal pathogen, which presents an emerging and global threat to healthcare facilities. C. auris is often resistant to multiple classes of antifungal agents – and this is on top of fungi being difficult to treat in the first place! C. auris is tricky to identify accurately from a diagnostic laboratory perspective, and is often mis-identified. C. auris is reported increasingly commonly as a cause of hospital outbreaks. For example, in the UK, large and high profile outbreaks have been identified at the Royal Brompton hospital in London and in Oxford. The global prevalence of C. auris is rising. This will be explained in part by more awareness of the organism from a laboratory point of view, and subsequently less misidentification of C. auris. However, perhaps due to the increase in global use of antifungal agents, it is also clear that prevalence is increasing.
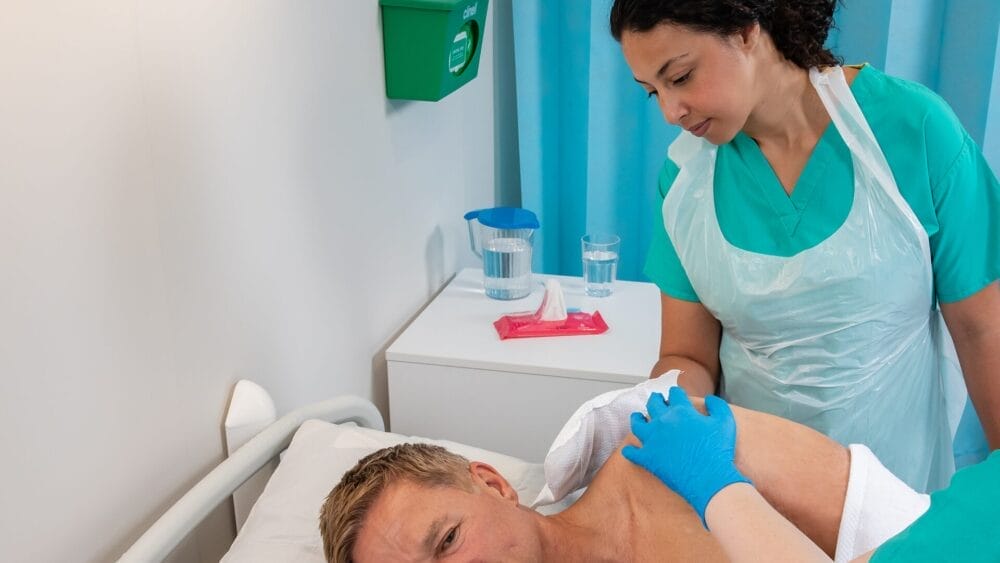
C. auris frequently colonises both the gastrointestinal tract and the skin of humans. This means that C. auris is shed into the environment, and results in widespread contamination of environmental surfaces, and the surfaces of shared medical equipment. C. auris has the capacity to survive on dry surfaces for weeks or longer. Part of this capability to surface on dry surfaces is linked to the ability to form dry surface biofilm. To top it all off from an environmental perspective, C. auris is also less susceptible to some disinfectants than other fungi.
National and international guidance for the prevention of the spread of C. auris in healthcare facilities recommend a range of infection prevention measures. This includes screening for C. auris in high risk patient groups (especially those with overseas hospitalisation), segregation of patients with C. auris from other patients, careful attention to hand hygiene, and disinfection of environmental surfaces and shared medical equipment.
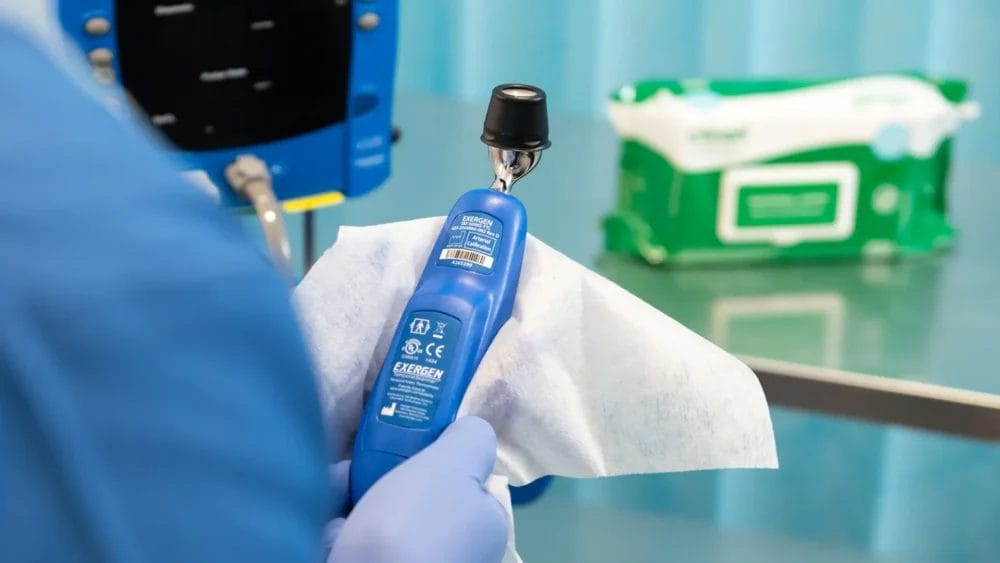
There are several infection prevention and control measures which can help combat the spread of C. auris. Below are some considerations (but not an exhaustive list).
– Frequent environmental decontamination with products which have proven efficacy against C. auris. It’s important to note that shared items of medical equipment have been implicated in C. auris outbreaks hence the need to regularly decontaminate the environment. Rooms should also be terminally cleaned following the discharge of C. auris infected or colonised patients and a consideration should be given to automated technologies such as UV-C.
– Chlorhexidine can be used to decontaminate the skin of patients who are colonised with C. auris. Whilst this will not ‘decolonise’ the patient, it will reduce the concentration of C. auris on the skin and some studies suggest this will reduce the risk of cross-transmission.
– Isolation of patients in a single patient room, ideally with ensuite facilities.
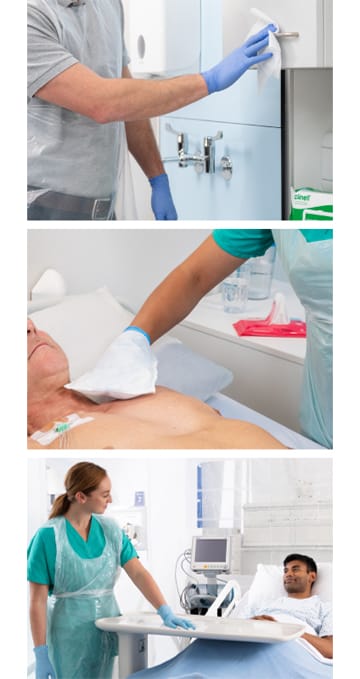
C. auris is an emerging pathogen globally. With limited treatment options for patients who are infected, preventing the spread of C. auris in healthcare settings is of paramount importance. The contaminated environment plays a key role in the spread of C. auris in healthcare settings, and effective decontamination of contaminated environmental surfaces is a vital part of any strategy to prevent the spread of C. auris.
SHARE THIS ARTICLE
Tags
Latest News
Embracing sustainability and cost savings: The journey of Clinell Indicator Notes to paper-based solutions
At GAMA Healthcare, we’ve always prided ourselves on being at…
Introducing HEXI HUB: A seamless transition in our product line
We’re pleased to announce an update to our product offering…
Innovative solutions for tackling Carbapenemase-producing Enterobacteriaceae (CPE) at King’s College Hospitals
King’s College Hospital NHS Foundation Trust, one of London’s largest…
Gloves Off: reducing unnecessary plastic waste during environmental cleaning and disinfection
In this blog, Dr Phil Norville discusses the momentum-gaining ‘Gloves…