Posted
28th February 2022
Research
This week’s article is a summary of the latest Global report published in the Lancet journal, on the effects of antimicrobial resistance (AMR), assessing a range of factors from number of deaths to hospitalisation which directly affects several of the global sustainability goals (SDGs). With an emphasis on efficient infection prevention and control in the hospitals, the report was jointly produced by the Bill & Melinda Gates foundation, Wellcome trust and Department of Health and Social Care.
Introduction
This study presented the first comprehensive global estimate of the burden of bacterial AMR covering an extensive survey of pathogens and pathogen-drug combinations using consistent methods for both counterfactual scenarios which are: Death attributed to AMR and deaths associated with AMR.
What is AMR? Brief overview and explanation
Antimicrobial resistance occurs when bacteria, viruses, fungi, and parasites evolve over time reducing the effect of medicine and making infections hander to treat, increasing the risk of disease. Bacterial antimicrobial resistance (AMR) remains a global and development threat, compromising treatment of the wildly diversifying scope of infections caused by viruses, bacteria, and fungi. Drug resistance is a natural biological mechanism but can be increased and accelerate by various factors such as poor infection control practise, misuse of medicines, global trade, and travel.
Findings from the Global AMR report?
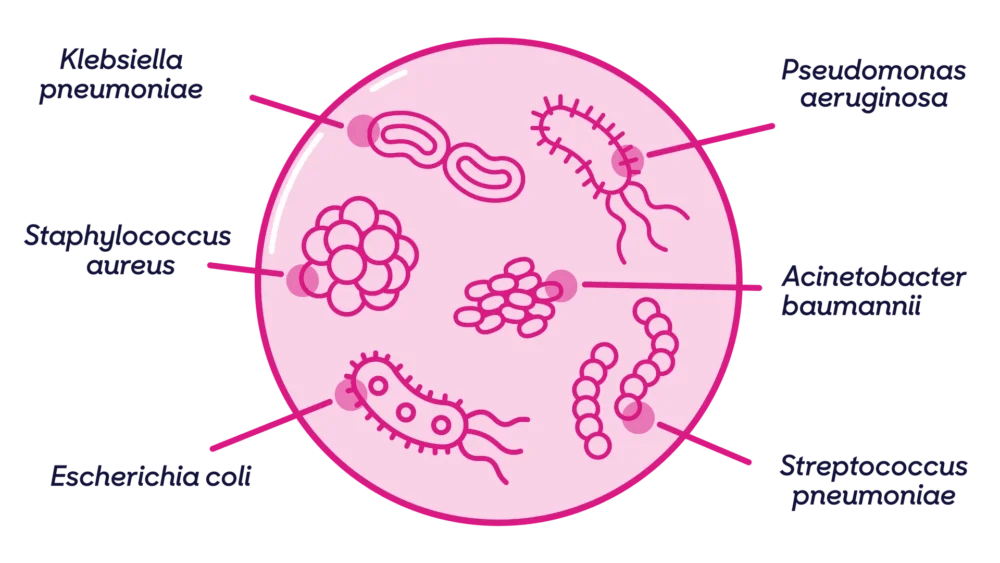
Being the most comprehensive report of its kind, the global AMR report attempted to estimate the deaths and disability-adjusted life year (DALYs) associated with bacterial AMR for 23 pathogen which included Staphylococcus aureus, drug-resistant tuberculosis Acinetobacter etc. It also included the surveillances of 88 pathogen-drug combination across 204 countries and territories in 2019. This information was acquired through systematic literature reviews, hospital systems and surveillance systems. Other data compositions were number of deaths related to infection, infection deaths attributable to a given infectious syndrome, infectious syndrome deaths attributed to a pathogen and percentage of pathogen resistant to antibiotic of interest and the excess risk of death or duration of infection associated with resistance.
The significant finding can be summarised into the following
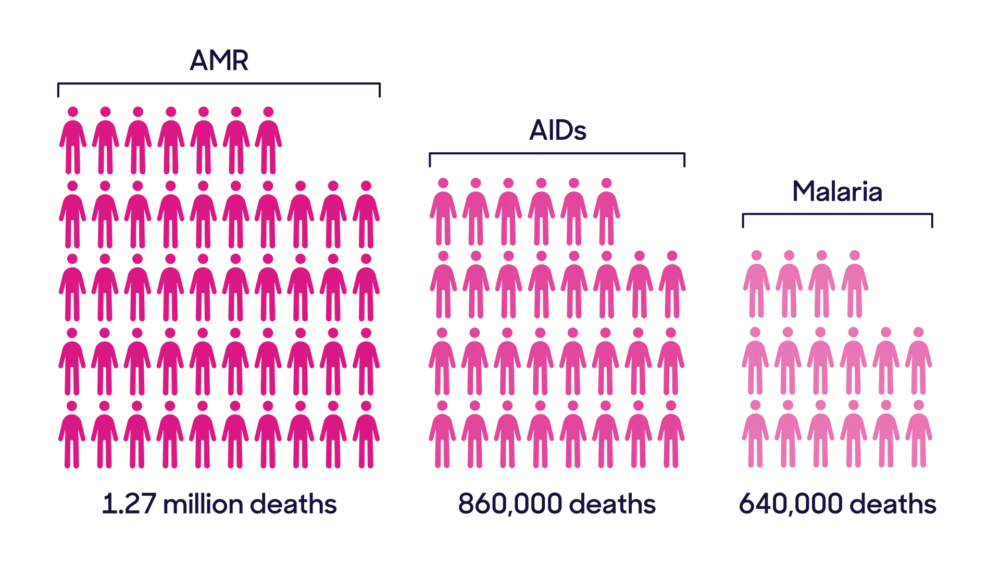
- Deaths: An estimated 4.95 million deaths are associated with bacterial AMR in 2019 with 929,000 deaths attributed to AMR globally.
- Health economics: Though no specific costs were stated the evidence showed on a regional level, the highest rate of deaths attributed to microbial resistance showed western sub-Saharan Africa at 27.3 deaths per 100,000 and the lowest in Australia with 6.5 deaths per 100, 000. This indicates a four times higher chance of death associated with pathogen infection based on regional resource. Highlighting the financial and educational disparities between high-income countries (HICs) and Low-income countries (LIC’s) which contributed to higher infection rates.
- Global deaths (counts) attributable to and associated with bacterial AMR by pathogens in 2019, highlighted Escherichia coli and Staphylococcus aureus as the highest contributors to global deaths caused by AMR infections.
This comprehensive assessment of the global burden of AMR, spotlights AMR rising global threat to the current practise of medicine and global health initiatives. Showing AMR as one of the leading cause of deaths globally, with the highest burden in low-resourced regions. The data calls into review location-specific policy, the need for new vaccinations, antibiotics and particularly infection prevention and control programmes.
Future proofing
Considering the scope of AMR effect on global health including the consistent evolution of microbes. Specific themes and enablers have been identified as solutions to this growing global threat:
- IPC: Infection prevention and control greatly impacts human drug-resistant infections directly by reducing the need for antimicrobials. In comparison to therapeutic treatments, vaccines and other diagnostic procedures, fundamental IPC interventions such as environmental decontamination, hand hygiene etc are more cost-effective. Prevention is better than cure, especially when there is none (i.e., antibiotics).
- Use of Antibiotics: Ensuring the human consumption of antibiotics and the wide use of these drugs are used appropriately reducing cost of inappropriate consumption.
- Vaccinations: To reduce the consumption of antibiotics, as a longer-term preventative, vaccinations can prevent infection and transmission in both humans and animals.
- Auditing & Surveillance: Using supporting tools such as the WHO’s guidance on country implementation of the Global Antimicrobial resistance surveillance system (GLASS). Knowing the overall extent AMR has and its development over time in different geographical locations.
Summary
Infection prevention and control (IPC) is a unique field focused on safety and quality of care. If the Global AMR report has taught us anything, is that now more than ever preventative measures must be prioritised including management strategy against the spread of drug-resistant pathogens. Over the years AMR has swiftly shifted from a largely technical topic to a mainstream political issue, which has spurred the need to globally challenge the misuse of antibiotics in medical care and in animals especially within regions with less surveillance. Which are often areas with less resources.
SHARE THIS ARTICLE
Tags
Latest News
Embracing sustainability and cost savings: The journey of Clinell Indicator Notes to paper-based solutions
At GAMA Healthcare, we’ve always prided ourselves on being at…
Introducing HEXI HUB: A seamless transition in our product line
We’re pleased to announce an update to our product offering…
Innovative solutions for tackling Carbapenemase-producing Enterobacteriaceae (CPE) at King’s College Hospitals
King’s College Hospital NHS Foundation Trust, one of London’s largest…
Gloves Off: reducing unnecessary plastic waste during environmental cleaning and disinfection
In this blog, Dr Phil Norville discusses the momentum-gaining ‘Gloves…