Posted
25th January 2022
Research
In this week’s article, our Clinical & Scientific Director, Dr. Phillip Norville, discusses the role of ventilation in mitigating the risk of SARS-CoV-2, alternative technologies to improve air hygiene and our latest innovation in air filtration, Rediair.
What is ventilation?
Put simply ventilation is a process which moves outdoor air into a room or building, diluting pollutants or contaminants from it. These pollutants are things such as dust, allergens and microorganisms. Ventilation from an IPC perspective has always played a role in good IPC practice as infectious microorganisms such as viruses and bacteria are expelled into the air when an infectious person coughs, talks or even just through breathing. Good ventilation can dilute the amount of microorganisms in the air, lowering the risk of transmission to others.
How do bacteria and viruses spread through the air?
Bacteria and viruses are spread through the air by small particles, termed aerosols and droplets. Aerosols are smaller than droplets and can remain suspended in the air for longer periods of time. Infectious aerosols above the infectious dose (the amount required to cause an infection) could be present after the discharge of an infectious patient for up to 26 hours (using the example of MERS-CoV), assuming no air changes in the room (Otter et al., 2016).
The role of ventilation in mitigating the risk of SARS-CoV-2
The COVID-19 pandemic has reinforced the importance of fundamental pillars of infection prevention and control (IPC) such as hand washing and environmental decontamination. There has also been focus on the role of ventilation in mitigating the risk of SARS-CoV-2 transmission, given that poorly ventilated areas may increase the risk of transmission. Ventilation is one example of where in the past two years we have seen significant changes and tweaks to elements of IPC guidance, highlighting the challenges healthcare staff and IPC teams across the world face from the consistently evolved threat poses by infectious microorganisms.
Related article: Omicron: why all the fuss?
Considering alternative technologies to improve air hygiene
The latest UK hospital guidance for SARS-CoV-2 and other respiratory viruses includes a recommendation to consider alternative technologies to improve air hygiene when ventilation is considered inadequate or cannot be assessed. Air filtration units offer a solution to overcome poor ventilation in such areas. By removing airborne particles, air filtration systems can reduce exposure by inhalation of infectious aerosols, deposition on susceptible mucous membranes or transfer to mucous membranes by contaminated hands.
View: Rediair our latest development in air filtration.
HEPA filters
Air filtration units typically employ high-efficiency particulate absorbing (HEPA) filters to remove pollutants from the air. These filters can capture small particles such as aerosols and droplets so are an ideal mechanism to remove infectious microorganisms from the air.
HEPA units are divided into 2 classes HEPA 13 and HEPA 14. A HEPA grade of H13 can remove 99.95% of all particles in the air measuring 0.3 microns in diameter, while a HEPA grade H14 removes 99.995%. The extra “9” might sound small, but it makes a big difference. It means H14 filters are 10x more effective than H13 filters, removing at least 99.995% of 0.3 µm sized particles from the air.
Tracking the impact of air filtration systems can be difficult as sampling microorganisms from the air (particularly viruses) is a difficult thing to assess. Several studies have utilised artificial methods to replicate aerosols movement and size in controlled conditions. An Australian study (employing glycerol to study aerosol movement) found that rooms equipped with mobile HEPA filtration units were 5 times faster at clearing aerosols in comparison to those without HEPA filters (Busing et al., 2021).
The impact of air filtration
We are starting to see research published around the impact of air filtration specifically on certain microorganisms. A crossover study in two COVID surge units conducted at Cambridge Hospital introduced air sampling units and portable HEPA filters. When the portable HEPA filters were introduced, SARS-CoV-2 was eliminated from the air. When the HEPA filters were removed, SARS-CoV-2 was once again detected in the air.
More evidence is required to demonstrate the benefits of air filtration on reducing the risk of transmission of infectious microorganisms but the importance of good ventilation is widely recognised and a topic that applies not only to healthcare facilities, but also offices and schools.

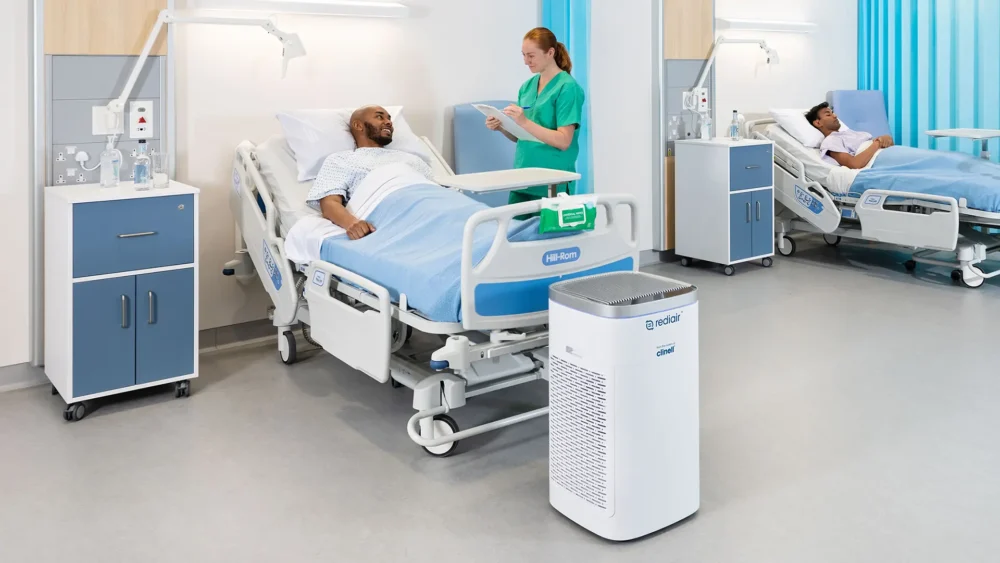
GAMA’s latest innovation in ventilation
We’re proud to announce the launch of Rediair, our latest innovation in ventilation. Rediair is an instant air purification device utilising dual HEPA 14 and carbon filters. These filters capture 10x the particles of a domestic HEPA 13 filter. Adaptable to any situation, Rediair has four different operating modes that begin to decontaminate the surrounding air within seconds, filtering out potential infectious microorganisms from the air.
If you’d like to find out more about the benefits of air filtration, visit our Rediair page. Alternatively, explore our latest development in patient isolation on our Rediroom page. Help us spread the word by sharing this article on social media.
SHARE THIS ARTICLE
Tags
Latest News
Embracing sustainability and cost savings: The journey of Clinell Indicator Notes to paper-based solutions
At GAMA Healthcare, we’ve always prided ourselves on being at…
Introducing HEXI HUB: A seamless transition in our product line
We’re pleased to announce an update to our product offering…
Innovative solutions for tackling Carbapenemase-producing Enterobacteriaceae (CPE) at King’s College Hospitals
King’s College Hospital NHS Foundation Trust, one of London’s largest…
Gloves Off: reducing unnecessary plastic waste during environmental cleaning and disinfection
In this blog, Dr Phil Norville discusses the momentum-gaining ‘Gloves…